You as the advanced practice nurse are working in a community health center. Your next patient is Mrs. Richards, a 39 year-old Caucasian female, presenting to the clinic with a history of Hypothyroidism, Depression, and recent history of Substance Abuse (Heroine Use). During the initial interview, it is revealed that her husband and two children were killed in a traffic accident 8 months ago and she reports using illicit drugs since their death.
Based on your knowledge of the Health Promotion Model, make a chart and/or diagram that outlines all components of the theory and how the theory can be applied to this case study to formulate a plan of care for this patient. Also, list one scholarly, practice-based resource (article and/or clinical guideline) that supports the application of the Health Promotion Model in clinical practice.
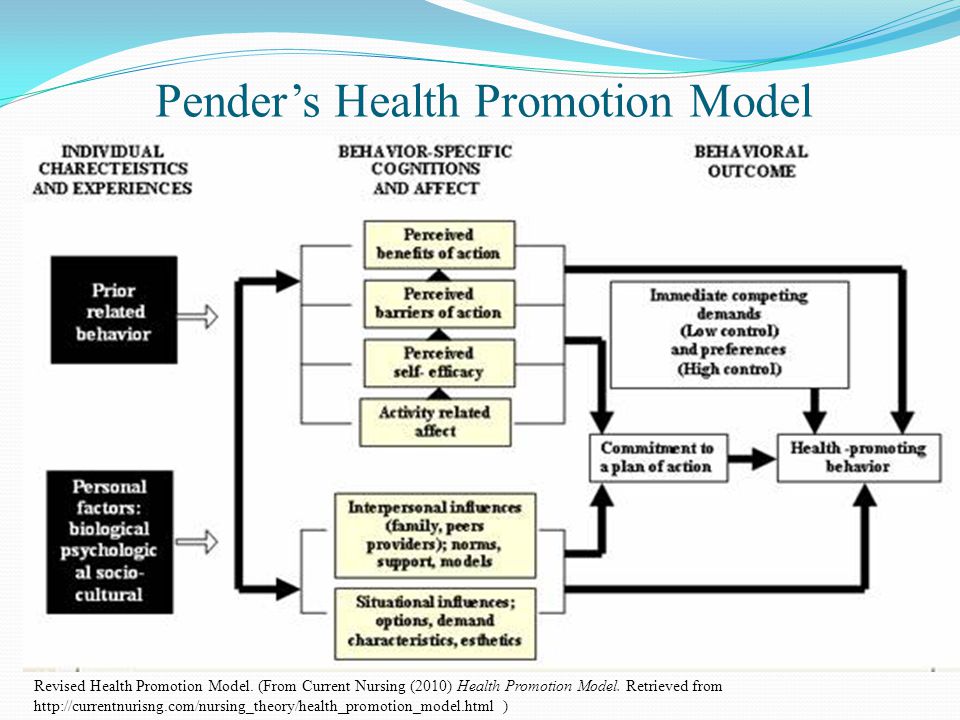
please see model attached.
http://www.nursing-theory.org/theories-and-models/pender-health-promotion-model.php
Delivering a high-quality product at a reasonable price is not enough anymore.
That’s why we have developed 5 beneficial guarantees that will make your experience with our service enjoyable, easy, and safe.
You have to be 100% sure of the quality of your product to give a money-back guarantee. This describes us perfectly. Make sure that this guarantee is totally transparent.
Read moreEach paper is composed from scratch, according to your instructions. It is then checked by our plagiarism-detection software. There is no gap where plagiarism could squeeze in.
Read moreThanks to our free revisions, there is no way for you to be unsatisfied. We will work on your paper until you are completely happy with the result.
Read moreYour email is safe, as we store it according to international data protection rules. Your bank details are secure, as we use only reliable payment systems.
Read moreBy sending us your money, you buy the service we provide. Check out our terms and conditions if you prefer business talks to be laid out in official language.
Read more